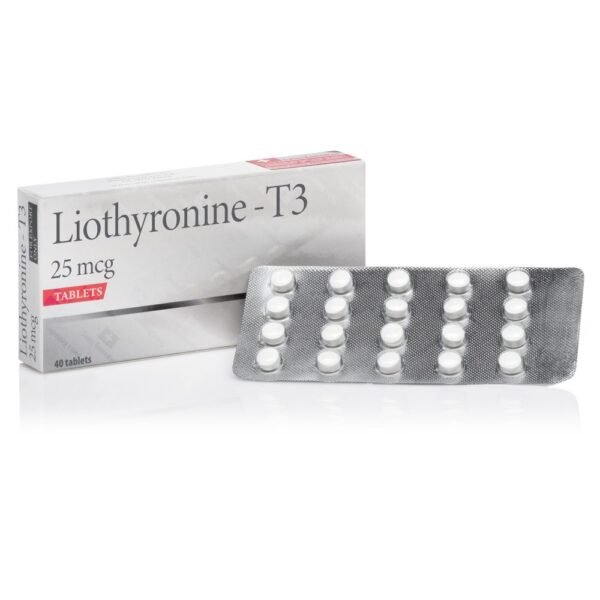
Buy Liothyronine T3 (CYTOMEL)
$50.00 – $70.00Price range: $50.00 through $70.00
Buy Liothyronine T3 without a prescription
Buy Liothyronine T3 (CYTOMEL) sodium 25 mcg and 5 mcg discreetly online without a prescription, safely and reliably through our online pharmacy .
Liothyronine T3 is a prescription medication used to treat the symptoms of low thyroid hormone (hypothyroidism),
enlarge thyroid (non-toxic goiter), myxedema, and myxedema coma. Cytomel can be use alone or with other medications.
Buy Liothyronine T3 without a prescription sodium tablets contain liothyronine (L-triiodothyronine or LT3), a synthetic form of a natural thyroid hormone, and are available as a sodium salt.
Buying 25 mcg of liothyronine is equivalent to approximately 1 grain of desiccated thyroid or thyroglobulin and 0.1 mg of L-thyroxine.
Each Liothyronine sodium tablet contains: 5 mcg deboss KPI and 115; 25 mcg scored and deboss KPI and 116; 50 mcg scored and debossed KPI and 117.
Inactive ingredients consist of calcium sulfate, gelatin, cornstarch, stearic acid, sucrose and talc.
Buy Liothyronine belongs to a class of medications call thyroid products.
Thyroid hormone medications
Thyroid hormone medications are natural or synthetic preparations containing tetraiodothyronine (T4, levothyroxine ) sodium or triiodothyronine (T3, liothyronine) sodium, or both.
T4 and T3 are produce in the human thyroid gland by iodination and coupling of the amino acid tyrosine.
T4 contains four iodine atoms and is formed by the combination of two molecules of diiodotyrosine (DIT).
T3 contains three iodine atoms and is form by the combination of one molecule of DIT with one molecule of monoiodotyrosine (MIT). Both hormones are store in the thyroid colloid as thyroglobulin.
Liothyronine Instructions
Thyroid hormone drugs are indicate:
As replacement or adjunctive therapy in patients with hypothyroidism of any etiology, except transient hypothyroidism during the recovery phase of subacute thyroiditis.
This category includes cretinism, myxedema, and simple hypothyroidism in patients of any age (pediatric, adult, elderly)
or condition (including pregnancy); primary hypothyroidism due to functional deficiency, primary atrophy, the partial or total absence of the thyroid gland,
or the effects of surgery, radiation, or drugs, with or without the presence of goiter; and secondary (pituitary) or tertiary (hypothalamic) hypothyroidism.
Liothyronine dosage
The dosage of thyroid hormones is determine by the indication and must in each case be individualized according to the patient’s response and laboratory findings.
Liothyronine sodium tablets are intended for oral administration; a once-daily dosage is recommend.
Although liothyronine sodium has a rapid onset of action, its metabolic effects persist for several days after discontinuation.
Mild hypothyroidism
The recommend starting dose is 25 mcg daily. The daily dose can then be increase by a maximum of 25 mcg every one or two weeks.
The usual maintenance dose is 25 to 75 mcg daily.
The rapid onset and dissipation of action of liothyronine sodium (T3), compare with levothyroxine sodium (T4),
has led some clinicians to favor its use in patients who may be more susceptible to the adverse effects of thyroid medication.
However, the wide fluctuations in serum T levels that follow its administration and the potential for more pronounced cardiovascular side effects tend to offset these reported advantages.
Liothyronine T3 sodium tablets can be used in place of levothyroxine (T4) during radioisotope scanning procedures, as the induction of hypothyroidism in these cases is abrupt and may be shorter-live.
They may also be preferred when impairment of peripheral T4 to T3 conversion is suspected.
Myxedema
The recommend starting dose is 5 mcg per day. This can be increase by 5 to 10 mcg every one or two weeks. Once 25 mcg is reach,
the dosage can be increased by 5 to 25 mcg every one or two weeks until a satisfactory therapeutic response is achieved.
The usual maintenance dose is 50 to 100 mcg daily.
Myxedema coma
Myxedema coma is usually precipitate in the hypothyroid patient by prolonge intercurrent illness or medications such as sedatives and anesthetics and should be consider a medical emergency.
An intravenous preparation of liothyronine sodium is recommend for use in Myxedema coma/precoma.
Congenital hypothyroidism
The recommend starting dose is 5 mcg per day, with a 5 mcg increase every 3 to 4 days until the desire response is achieved.
Infants a few months old may only need 20 mcg per day for maintenance.
For children under 1 year of age, 50 mcg daily may be require. After 3 years of age, a full adult dose may be necessary.
Simple stioner
The recommended starting dose is 5 mcg per day.
This dose can be increase by 5 to 10 mcg every one or two weeks. Once the daily dose reaches 25 mcg, the dose can be increase by 12.5 or 25 mcg every one or two weeks.
The usual maintenance dose is 75 mcg daily.
In the elderly or pediatric patients, therapy should be initiated at 5 mcg daily and increased only by 5 mcg increments at the recommend intervals.
Liothyronine Drug Interactions
Oral anticoagulants
Thyroid hormones appear to increase the catabolism of vitamin K-dependent clotting factors.
If oral anticoagulants are also administer, the compensatory increase in clotting factor synthesis is impaired.
Patients stabilize on oral anticoagulants who prove to require thyroid replacement therapy should be closely monitor when starting thyroid replacement therapy.
If a patient is truly hypothyroid, a reduction in the anticoagulant dosage is likely necessary.
No special precautions appear necessary when initiating oral anticoagulant therapy in a patient already stabilize on maintenance lymph node therapy.
Insulin or oral hypoglycemics
Initiating thyroid replacement therapy may increase insulin or oral hypoglycemic requirements.
The observe effects are poorly understood and depend on several factors, such as the dose and type of thyroid preparation, and the patient’s endocrine status.
Patients receiving insulin or oral hypoglycemic agents should be closely monitored during the initiation of thyroid replacement therapy.
Cholestyramine
Cholestyramine binds both T4 and T3 in the intestine, impairing the absorption of these thyroid hormones.
In vitro studies indicate that the binding is not easily remove.
Therefore, 4 to 5 hours should elapse between the administration of cholestyramine and thyroid hormones.
Tricyclic antidepressants
Using thyroid products with imipramine and other tricyclic antidepressants can increase receptor sensitivity and enhance antidepressant activity; transient cardiac arrhythmias have been observe.
Thyroid hormone activity may also be enhance.
Digitalis
Thyroid preparations can enhance the toxic effects of digitalis.
Thyroid hormone replacement increases the metabolic rate, necessitating an increased digitalis dosage.
Ketamine
When administer to patients receiving thyroid preparation, this parenteral anesthetic may cause hypertension and tachycardia.
Use with caution and be prepare to treat hypertension if necessary.
Vasopressors
Thyroxine increases the adrenergic effect of catecholamines such as epinephrine and norepinephrine. Therefore, injecting these agents into patients receiving thyroid preparations increases the risk of precipitated coronary insufficiency, especially in patients with coronary artery disease. Careful observation is required.
Liothyronine T3 side effects
T3 Liothyronine sodium can cause serious side effects, including:
- headache;
- irritability;
- Trouble sleeping;
- Nervousness;
- increased sweating;
- heat intolerance;
- diarrhea and menstrual changes;
- nausea.
Liothyronine T3 overdose
Headache, irritability, nervousness, sweating, arrhythmia (including tachycardia), increased intestinal motility, and menstrual irregularities may occur. Angina pectoris or congestive heart failure may be induced or exacerbated. Shock may also develop.
Massive overdose can lead to symptoms similar to thyroid storm. Chronic excessive dosing will produce the signs and symptoms of hyperthyroidism.
Liothyronine Contraindications
Thyroid hormone preparations are generally contraindicated in patients with diagnosed but as yet uncorrected adrenal cortical insufficiency, untreated thyrotoxicosis and apparent hypersensitivity to any of their active or foreign components.
There is, however, no well-documented evidence from the literature of true allergic or idiosyncratic reactions to thyroid hormone.
| DOSE | 25 mcg, 5 mcg |
|---|
Related products
Buy Steroids
Buy Steroids
Buy Steroids
Buy Steroids
Buy Steroids
Buy Steroids
Buy Steroids
Buy Steroids